Feline Lymphoma - Cats are Not Small Dogs
- Jun 29, 2017
- 4 min read

Lymphoma accounts for at least one third of all feline cancers. Compared to dogs, there are different causes of lymphoma development in cats, cats do not present with generalized lymph node enlargement, and cats may receive a form of treatment other than combination chemotherapy.
So what causes the development of lymphoma in cats? Infections with either the feline leukemia virus (FeLV) or the feline immunodeficiency virus (FIV) will increase a cat’s chance of developing lymphoma. Other factors that have been found to increase a cat’s risk of the disease are exposure to tobacco smoke, chronic inflammation, and immunosuppressive therapy after a cat has received a kidney transplant.
The classification of feline lymphoma is based on the area of the body that is affected. The types of lymphoma in the cat include: gastrointestinal/alimentary (stomach and intestines), mediastinal (area in the chest in front of the heart), nasal (nose), multicentric (multiple enlarged lymph nodes), and renal (kidneys). As with dogs, all areas of the body are susceptible to lymphoma, and other areas that can be affected include the eyes, brain and spinal cord, and the skin. Interestingly, cats that have renal lymphoma will often develop central nervous system (CNS) involvement, and it appears fairly common that cats with nasal lymphoma will also have renal involvement.
Cats that are infected with FeLV tend to develop lymphoma at a young age, and the eyes, kidneys, mediastinum, and central nervous system are most often affected. The intestines and nose are more commonly affected with lymphoma in cats that are older and do not have an FeLV infection. Besides the locations, a cat’s lymphoma will also be classified as high or low grade, based on the size of cells present. High grade lymphomas are aggressive cancers that are made up of large lymphocytes (similar to the disease that develops in dogs) while low grade lymphomas often have a slowly progressive course and are made up of small lymphocytes.
The clinical symptoms that a cat with lymphoma may exhibit vary greatly based on the location of the disease. With mediastinal lymphoma, the cat will often develop fluid in the chest (known as pleural effusion), which makes breathing difficult. (As a side note, cats don’t pant like dogs, so if you see that your cat is breathing with its mouth open please contact your veterinarian immediately as this can be a sign of a serious medical condition!) The common signs that you may see include open mouth breathing, a bluish or gray tinge to the gums or tongue, fast breathing, or “abdominal breathing” in which the cat is has exaggerated motion in their abdominal muscles to try and expand the lungs. Cats with nasal lymphoma will often have a swelling over the nose or face and nasal discharge. Cats are also prone to upper airway infections, which can also cause a discharge from the nose; however, these types of infections are not likely to cause the discharge to be only blood or blood tinged. If you see any type of bloody discharge from the nose, it is another situation that you should schedule an exam with your veterinarian as soon as possible.
X-ray of a cat with mediastinal lymphoma
The most common signs of intestinal lymphoma in cats are unexplained weight loss, a decrease in appetite, vomiting, and diarrhea. Virtually any sign of a generalized illness can be present in a cat with multicentric lymphoma. As this is the form similar to the disease in dogs, you may also feel lumps on the body in the areas where the lymph nodes are located (refer to my blog on canine lymphoma for a visual). Cats with renal lymphoma may have a mass that can be felt in the belly, or they may have blood in the urine, increased thirst, and increased urine output.
Diagnosing lymphoma in a cat is often more difficult than in a dog. However, cats with multicentric or renal lymphoma can often be diagnosed with a fine needle aspirate and those with mediastinal lymphoma can be diagnosed with a fine needle aspirate, or examination of the fluid present in the chest. For the other locations, a fine needle aspirate will likely be inadequate. A CT scan with biopsies is essential to diagnose cats with nasal lymphoma, and an ultrasound (sonogram) exam of the abdomen with either endoscopic or surgical biopsies will be needed to diagnose a cat with intestinal lymphoma.

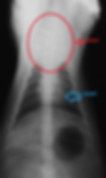
X-ray of a cat with lymphoma of the kidney
I’m sure you will be surprised to learn that the type of treatment offered, and the anticipated life span will depend on the area of the body that is affected with the disease. Cats with renal, multicentric, and mediastinal lymphoma will benefit most from a multi-agent chemotherapy protocol. The chance of response can be as high as 70%, but is unfortunately often less than 50%. Life expectancy for these cats are approximately 3-6 months. Cats with intestinal lymphoma respond very well to minimal chemotherapy treatment. Treatment with chlorambucil (Leukeran®), an oral chemotherapy drug, often causes remission in the majority of cats. We expect these cats to live 18 months on average, and when they come out of remission, changing their chemotherapy to cyclophosphamide (Cytoxan®), also an oral chemotherapy drug, will often result in a second remission and extend their life an additional 6 months. Cats with nasal lymphoma have the best response to radiation therapy, and their average life span is more than 18 months. The addition of a multi-agent chemotherapy protocol is recommended for cats that have kidney involvement. Some of these cats will have lymphoma recur somewhere outside of the nose, and these cats will also benefit from a multi-agent chemotherapy protocol.
So now we know about lymphoma in dogs and cats. In the next blog, we will continue to discuss specific tumors. I think we will cover leukemia in dogs and cats. Are there any specific cancers that you would like me to write about? If so, let us know in the comment section!





















